 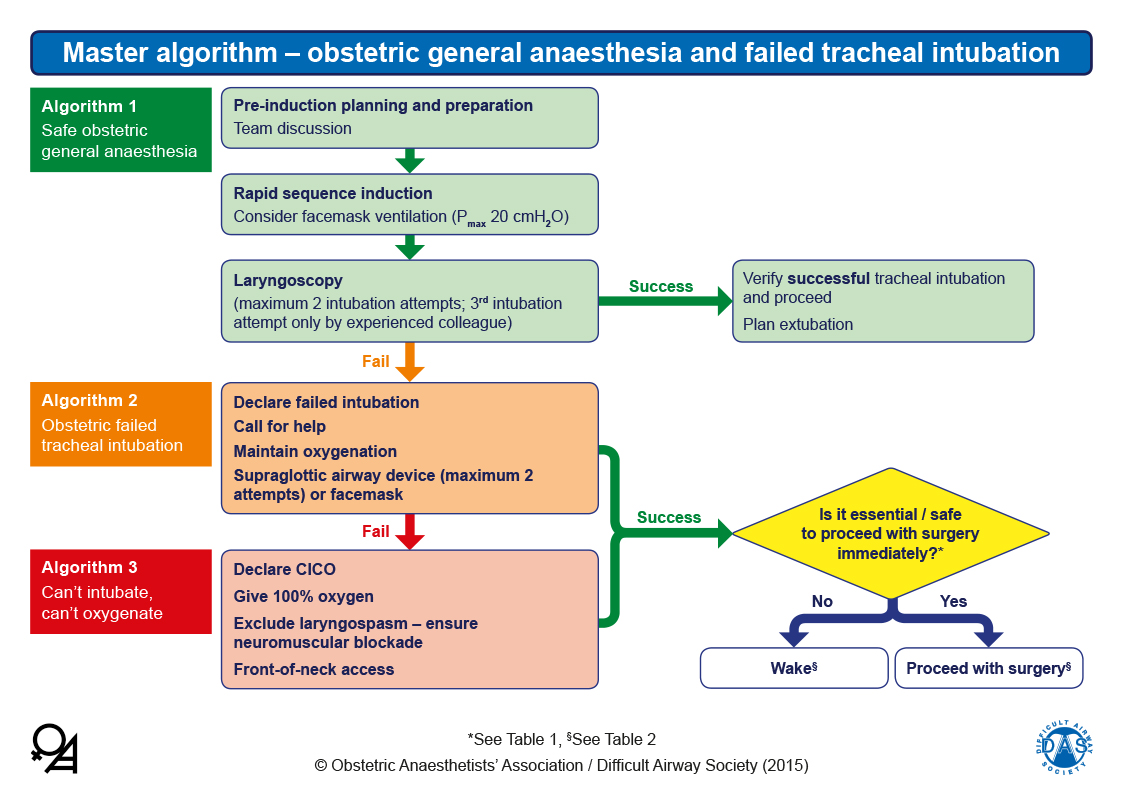
Most of the airway guidelines discuss either the unanticipated or both the unanticipated and anticipated difficult airway. As such, clinicians who perform tracheal intubation must have pre-planned airway strategies, and be trained and be competent in the airway devices and techniques involved in difficult airway management. In one large database, less than 2% of registered cases were difficult tracheal intubations, and yet 93% of these were unanticipated. Extubation following difficult tracheal intubation is beyond the remit of this article, and is not discussed. These are henceforth collectively termed the ‘airway guidelines’ (Table 1). The remaining nine articles were from the Canadian Airway Focus Group (CAFG), France’s Société Française d’Anesthésie et de Réanimation (SFAR), the German Society for Anesthesiology and Intensive Care Medicine (DGAI), the All India Difficult Airway Association (AIDAA), the Japanese Society of Anesthesiologists (JSA), the Scandinavian Society of Anesthesiology and Intensive Care Medicine (SSAI), the American Society of Anesthesiologists (ASA) and the United Kingdom’s Difficult Airway Society (DAS). We excluded articles pertaining to out-of-theater or pre-hospital settings (2 articles) and those related to obstetric patients (2 articles) and critical care/intensive care patients (3 articles). We extracted guidelines or consensus statements on adult difficult tracheal intubation from anesthetic societies. We used the search terms (‘anesthesia’ OR ‘anesthesiology’ OR ‘anesthesia’ OR ‘anesthesiology”) AND (‘‘guidelines’) AND (‘airway’ OR ‘intubation’). We obtained difficult tracheal intubation guidelines by performing a PubMed database search for peer-reviewed English language articles published between 01 January 2010 and 01 January 2020. Valuing, and a greater understanding of, these differences and modifications may lead to greater adherence to the new COVID-19 guidelines. We combine the principles from both sets of guidelines and explain the necessary modifications to the airway guidelines, to form a failed tracheal intubation airway strategy in the COVID-19 patient. 
Our article identifies and compares pre-pandemic difficult airway guidelines with the recent anesthetic COVID-19 guidelines. In turn, most of the anesthetic COVID-19 guidelines do not, or only briefly, discuss an airway strategy after failed tracheal intubation. These difficult airway guidelines require modifications in order to align with the principles of the anesthetic COVID-19 guidelines. Pre-pandemic difficult airway guidelines include those from Canada, France, Germany, India, Japan, Scandinavia, the United States and the United Kingdom. Hospitalized COVID-19 patients may require airway interventions, and difficult tracheal intubation secondary to laryngeal edema has been reported. These guidelines originate from Australia and New Zealand, Canada, China, India, Italy, Korea, Singapore, the United States and the United Kingdom. Many anesthethetic COVID-19 guidelines have emerged, whose underlying management principles include minimizing aerosol contamination and protecting healthcare workers. This may place anesthetists at higher risk of infection due to their frequent involvement in aerosol-generating airway interventions. 
The coronavirus disease 2019 (COVID-19) pandemic is caused by a coronavirus that is transmitted primarily via aerosol, droplets or direct contact. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
